Chinese Journal of Tissue Engineering Research ›› 2017, Vol. 21 ›› Issue (10): 1495-1500.doi: 10.3969/j.issn.2095-4344.2017.10.004
Previous Articles Next Articles
Guided bone regeneration membrane tube made of nano-hydroxyapatite/multi(amino acid) copolymer in the repair of large segmental bone defects
Yang Hong-sheng, Cao Zong-rui, Yan Xiao-hu, Li Yu-gang, Xu Ze-chuan, Chang Shan
- Department of Spinal Surgery, the First Affiliated Hospital of Chengdu Medical University, Chengdu 610500, Sichuan Province, China
-
Received:2017-01-10Online:2017-04-08Published:2017-05-08 -
Contact:Chang Shan, Master, Chief physician, Professor, Department of Spinal Surgery, the First Affiliated Hospital of Chengdu Medical College, Chengdu 610500, Sichuan Province, China -
About author:Yang Hong-sheng, Master, Attending physician, Department of Spinal Surgery, the First Affiliated Hospital of Chengdu Medical University, Chengdu 610500, Sichuan Province, China -
Supported by:a grant from Sichuan Provincial Department of Education, No. CYZ12-008, 13ZB0232; a grant from Sichuan Provincial Health and Family Planning Commission, No. 130395
CLC Number:
Cite this article
Yang Hong-sheng, Cao Zong-rui, Yan Xiao-hu, Li Yu-gang, Xu Ze-chuan, Chang Shan . Guided bone regeneration membrane tube made of nano-hydroxyapatite/multi(amino acid) copolymer in the repair of large segmental bone defects[J]. Chinese Journal of Tissue Engineering Research, 2017, 21(10): 1495-1500.
share this article
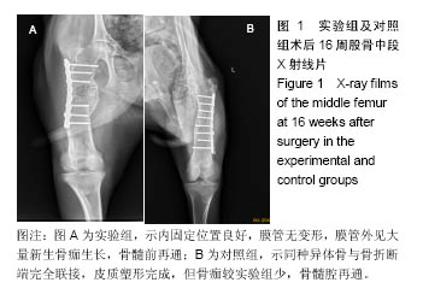
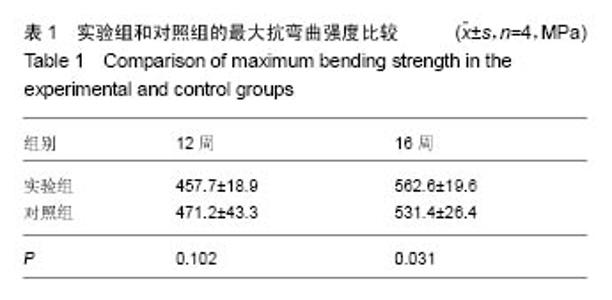
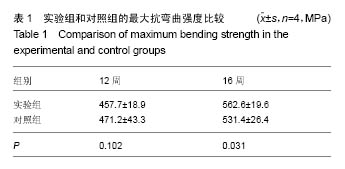
2.1 参与者数量分析 32只山羊随机分为2组,所有实验动物术后均成活良好,无意外死亡,伤口愈合良好,无红肿、积液、感染,术后10-12 d全部拆线。无手术后再骨折,内固定系统无移位、断裂等情况。 2.2 X射线观察结果 术后4周,实验组膜管与股骨接触两端可见较为均匀的云雾状密度影,膜管无塌陷移位;对照组同种异体骨管两端也可见云雾密度影,但实验组更为明显。 术后8周,实验组膜管外有明显骨痂生长、膜管内出现较多均匀密度影,膜管无异常;对照组同种异体骨管密度稍降低、骨管两端骨折线模糊、管内出现不均匀密度影。 术后12周,实验组膜管表面骨痂继续生长、增厚,骨缺损区内密度增加,两端可见呈帽状生长的骨皮质密度影,膜管位置良好,无移位;对照组骨痂生长较8周时稍增多,异体骨管两端与宿主骨开始融合,异体骨管密度有所增加。 术后16周,实验组股骨中段大量骨痂生长,骨痂包裹于膜管及钢板周围膜管与股骨连成整体,骨痂呈皮质骨样密度影像;对照组移植骨与宿主骨已完全连接,骨髓腔再通,整体塑形良好,对照组整体外骨痂量明显较实验组少(图1)。 "
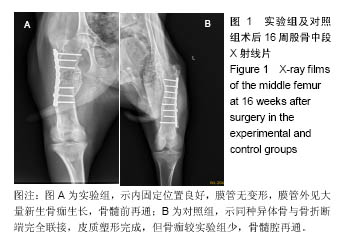
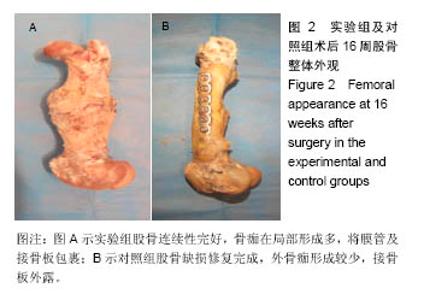
2.3 大体标本观察结果 实验组和对照侧动物各时间段被处死后观察,植入物周围无化脓、积液或坏死等迹象。 术后4周,实验组及对照组骨缺损两端有少量骨痂形成,膜管及同种异体骨管未被包裹,均与山羊股骨边界清楚,无明显连接。膜管及骨管均无塌陷、移位,管腔内外可见机化的血肿。 术后8周,实验组膜管内外均有见大量骨痂生长,以两端最明显,有部分骨痂开始向膜管表面爬行,膜管位置良好,管腔内有软骨样组织形成。对照组同种异体骨管外表面有较多骨痂生长,但异体骨段仍然未于股骨连接,管腔内成骨不明显。 术后12周,实验组膜管表面骨痂大量生长,膜管及接骨板完全被包裹,且骨痂在局部形成突起,膜管、骨痂与股骨连成整体,骨痂呈皮质骨硬度。对照组骨管表面少量骨痂形成,整体外骨痂量明显较实验组少,异体骨段与股骨靠骨痂连接。 术后16周,实验组膜管表面骨痂较12周更多,膜管内外均有再生皮质骨将缺损两端相互连接;对照组移植骨与宿主骨已完全连接,骨髓腔再通,骨痂塑形良好,但整体外骨痂形成较实验组少(图2)。"
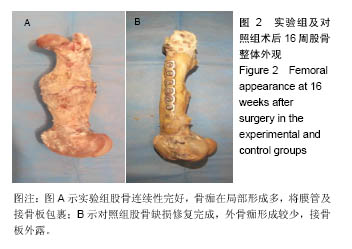
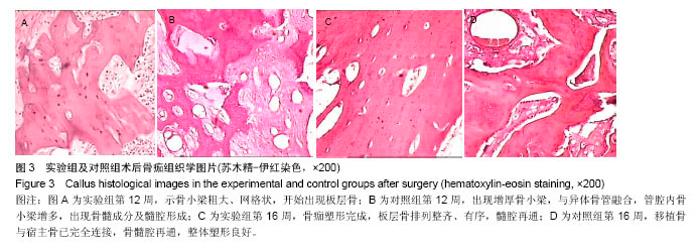
2.4 骨痂组织学观察 术后4周,实验组膜管桥接端开始出现肉芽组织及新生细小骨小梁。骨小梁成骨细胞增生活跃,间质中肉芽组织血管丰富,管腔内见陈旧性机化血凝块组织及新生毛细血管形成。对照组同种异体骨管内外均有肌纤维结缔组织长入。骨管开始出现骨吸收陷窝,陷窝内见肉芽组织形成及新生骨小梁长入,骨管内见新生肉芽组织形成。 术后8周,实验组膜管外见大量骨痂形成,骨小梁增粗,间质开始纤维化,并出现新生软骨细胞岛及软骨内成骨现象,膜管内部见纤维骨痂形成;对照组,同种异体骨管管壁骨吸收增多,新生骨小梁长入,异体骨管腔内外见新生骨小梁。 术后12周,实验组膜管外见大量骨性骨痂,骨小梁粗大成网格状,骨痂开始塑形成板层骨,板层骨排列紊乱、无序,膜管内骨小梁形成,间质出现新生骨髓成分及髓腔形成,膜管与内外骨痂紧靠但无明显连接(图3A);对照组骨小梁增厚,与异体骨管融合,管腔内骨小梁增多,骨髓腔再通(图3B)。 术后16周,实验组膜管外骨板形成、塑形,板层骨排列整齐、有序,膜管内骨断端有不规则骨形成,髓腔再通(图3C);对照组移植骨与宿主骨已完全连接,骨髓腔再通,整体塑形良好(图3D)。"
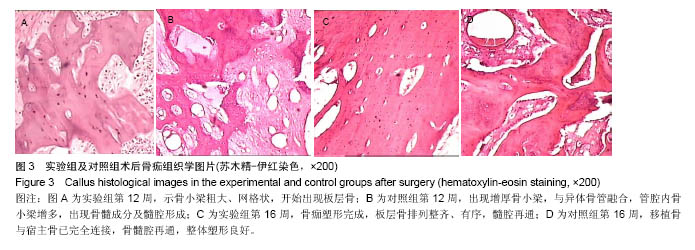
| [1]Chen FM, Zhang J, Zhang M,et al. A review on endogenous regenerative technology in periodontal regenerative medicine. Biomaterials. 2010;3: 7892-7927.[2]Geurs NC, Korostoff JM, Vassilopoulos PJ, et al. Clinical and histologic assessment of lateral alveolar ridge augmentation usinga synthetic long term bioabsorbable membrane and an allograft. J Periodontol. 2008;79(7):1133-1140.[3]Kaigler D, Avila G, Wisner-Lynch L, et al. Platelet-Derived Growth Factor Applications in Periodontal and Peri-Implant Bone Regeneration. Exp Opin Biol Ther. 2011;11(3): 375-385.[4]Navarro M, Valle S, Martinez S, et al. New macroporous calcium phosphate glass ceramic for guided bone regeneration. Biomaterials. 2004;25:4233-4241.[5]Verschueren DS, Gassner R, Mitchell R, et al. The effects of guided tissue regeneration (GTR) on modified Le Fort I osteotomy healing in rabbits. Int J Oral Maxillo Fac Surg. 2005;34(6):650-655.[6]侯劲松, 黄洪章,李祖兵.胚胎骨引导骨再生膜下植入对颌骨缺损修复的意义[J].现代口腔医学杂志, 2001, 15 (1):14.[7]Zakaria O, Madi M, Kasugai S. A novel osteogenesis technique: The expansible guided bone regeneration.J Tissue Eng. 2012;3(1):1-10.[8]Stevens B, Yang Y, Mohandas A,et al. A review of materials, fabrication methods,and strategies usedto enhance boneregeneration in engineered bone tissues.Biomed Mater Res B Appl Biomater. 2008; 85(2):573-582.[9]Fang TD, Nacamuli RP, Song HJ,et al.Guided tissue regeneration enhances bone formation ina rat model of failedsteogenesis.Plast Reconstr Surg. 2006;117(4):1177-1185. [10]Gugala Z, Lindsey RW, Gogolewski S. New Approaches in the Treatment of Critical-Size Segmental Defects in Long Bones. Macromol Symp. 2007;253:147-161.[11]Dalin C, Linde A, Gottlow J, et al. Healing of guided tissue regeneration. Plastic Reconstr Surg. 1988;81:672-676.[12]Kong L, Ao Q, Wang A, et al. Preparation and characterization of a multilayer biomimetic scaffold for bone tissue engineering. J Biomater.2007;22(3):223-239.[13]Gutta R, Baker RA, Bartolucci AA, et al. Barrier membranes used for ridge augmentation: is there an optimal pore size? J Oral Maxillofac Surg.2009;67(6):1218-1225.[14]Hong KS, Kim EC, Bang SH, et al. Bone regeneration by bioactive hybrid membrane containing FGF2 within rat calvarium. J Biomed Mater Res A. 2010;94(4):1187-1194.[15]Kikuchi M, Koyama Y, Yamada T, et al. Development of guided bone regeneration membrane composed of ß-tricalcium phosphate and poly(l-lactide-co-glycolide-co-e-caprolatone) composites. Biomaterials. 2004;25(28):5979-5986.[16]Jung RE, Windisch SI, Eggenschwiler AM, et al. A randomized-controlled clinical trial evaluating clinical and radiological outcomes after 3 and 5 years of dental implants placed in bone regenerated by means of GBR techniques with or without the addition of BMP-2. Clin Oral Implants Res. 2009;20(7):660-666.[17]段宏,沈彬,王光林,等.缓释碱性成纤维细胞生长因子微球对膜引导性骨再生的作用[J]. 中华实验外科杂志, 2004,21(12): 1526-1528.[18]Lindfors LT, Tervonen EA, Sándor GK, et al. Guided bone regeneration using a titanium-reinforced ePTFE membrane and particulate autogenous bone: the effect of smoking and membrane exposure. Oral Surg. Oral Med. Oral Pathol Oral Radiol Endod. 2010;109(6):825-830.[19]Kobbe P, Tarkin IS, Frink M, et al. Voluminous bone graft harvesting of the femoral marrow cavity for autologous transplantation: An indication for the“Reamer-Irrigator- Aspirator” ( RIA-) technique. Unfallchirurg. 2008;111(6): 469-472.[20]Sculean A, Nikolidakis D, Schwarz F.Regeneration of periodontal tissues: combinations of barrier membranes and graftingmaterials - biological foundation and preclinical evidence: a systematic review. J Clin Periodontol. 2008;35(8):106-116.[21]Kaigler D, Avila G, Wisner-Lynch L, et al. Platelet-Derived Growth Factor Applications in Periodontal and Peri-Implant Bone Regeneration. Expert Opin Biol Ther. 2011;11(3): 375-385.[22]Liu J, Kerns DG. Mechanisms of Guided Bone Regeneration: A Review. Open Dent J. 2014;8(1): 56-65.[23]Kim BS, Park KE, Kim MH, et al. Effect of nanofiber content on bone regeneration of silk fibroin/poly(ε-caprolactone) nano/microfibrous composite scaffolds. Int J Nanomedicine. 2015;10(9): 485-502.[24]Al-Hezaimi K, Ramalingam S, Al-Askar M, et al. Real-time-guided bone regeneration around standardized critical size calvarial defects using bone marrow-derived mesenchymal stem cells and collagen membrane with and without using tricalcium phosphate: an in vivo micro-computed tomographic and histologic experiment in rats. Int J Oral Sci. 2016;8(1): 7-15.[25]Li H , Yang L , Dong X , et al. Composite scaffolds of nano calcium deficient hydroxyapatite/multi-(amino acid) copolymer for bone tissue regeneration. J Mater Sci Mater Med. 2014; 25(5):1257-1265.[26]Yao Q, Ye J, Xu Q, et al.Composite scaffolds of dicalcium phosphate anhydrate /multi-(amino acid) copolymer: in vitro degradability and osteoblast biocompatibility. J Biomater Sci Polym Ed. 2015;26(4):211-223.[27]Duan H, Yang H , Xiong Y, et al. Effects of mechanical loading on the degradability and mechanical properties of the nanocalcium-deficient hydroxyapatite-multi(amino acid) copolymercomposite membrane tube for guided bone regeneration. Int J Nanomed. 2013;8(5):2801-2807.[28]Urban IA , Lozada JL , Wessing B , et al. Vertical Bone Grafting and Periosteal Vertical Mattress Suture for the Fixation of Resorbable Membranes and Stabilization of Particulate Grafts in HorizontalGuided Bone Regeneration to Achieve More Predictable Results: A Technical Report. Int J Periodontics Restorative Dent. 2016;36(2):153-159. [29]D'Elía NL , Mathieu C, Hoemann CD, et al. Bone-repair properties of biodegradable hydroxyapatite nano-rod superstructures.Nanoscale. 2015;7(44):18751-18762.[30]Karahalilo?lu Z, Ercan B, Taylor EN, et al. Antibacterial Nanostructured Polyhydroxybutyrate Membranes for Guided Bone Regeneration. J Biomed Nanotechnol. 2015;11(12): 2253-2263.[31]Simion M , Ferrantino L , Idotta E , et al. The Association of Guided Bone Regeneration and Enamel Matrix Derivative for Suprabony Reconstruction in the Esthetic Area: A Case Report. Int J Periodontics Restorative Dent. 2015;35(6):767-772. [32]Srivastava S, Tandon P, Gupta KK,et al. A comparative clinico-radiographic study of guided tissue regeneration with bioresorbable membrane and a composite synthetic bone graft for the treatment of periodontal osseous defects.J Indian Soc Periodontol. 2015;19(4):416-423.[33]Shim JH, Yoon MC, Jeong CM, et al.Efficacy of rhBMP-2 loaded PCL/PLGA/β-TCP guided bone regeneration membrane fabricated by 3D printing technology for reconstruction of calvaria defects in rabbit.Biomed Mater. 2014;9(6):065006.[34]Kim JY, Yang BE, Ahn JH,et al .Comparable efficacy of silk fibroin with the collagen membranes for guided bone regeneration in rat calvarial defects. J Adv Prosthodont. 2014;6(6):539-546.[35]Seok H, Kim MK, Kim SG, et al.Comparison of silkworm- cocoon-derived silk membranes of two different thicknesses for guided bone regeneration. J Craniofac Surg. 2014;25(6): 2066-2069.[36]杨晓波,裴福兴,严永刚,等.聚氨基酸复合纳米羟基磷灰石的体内生物相容性实验研究[J],中国矫形外科杂志, 2010,18(21):1809-1813.[37]Shimazaki Y , Takatsu Y. Combined Method of Immunoaffinity Membrane Within Tubes and MALDI-TOF MS for Capturing and Analyzing Amyloid Beta. Appl Biochem Biotechnol. 2015; 177(7):1565-1571.[38]Li H, Gong M, Yang A, et al. Degradable biocomposite of nano calcium-deficient hydroxyapatite-multi(amino-acid) copolymer. Int J Nano Med. 2012;7(8):1287-1295. [39]Qi XT, Li H, Qiao B, et al. Development and characterization of an injectable cement of nano calcium-deficient hydroxyapatite/ multi(amino acid)copolymer/calcium sulfate hemihydrate for bone repair. Int J Nanomedicine. 2013;8(21): 4441-445. |
| [1] | Xu Xinzhong, Wu Zhonghan, Yu Shuisheng, Zhao Yao, Xu Chungui, Zhang Xin, Zheng Meige, Jing Juehua. Biomechanical analysis of different ways of inserting Steinmann Pins into the femoral head [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1313-1317. |
| [2] | Wei Guoqiang, Li Yunfeng, Wang Yi, Niu Xiaofen, Che Lifang, Wang Haiyan, Li Zhijun, Shi Guopeng, Bai Ling, Mo Kai, Zhang Chenchen, Xu Yangyang, Li Xiaohe. Biomechanical analysis of non-uniform material femur under different loads [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1318-1322. |
| [3] | Yao Xiaoling, Peng Jiancheng, Xu Yuerong, Yang Zhidong, Zhang Shuncong. Variable-angle zero-notch anterior interbody fusion system in the treatment of cervical spondylotic myelopathy: 30-month follow-up [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(9): 1377-1382. |
| [4] | An Weizheng, He Xiao, Ren Shuai, Liu Jianyu. Potential of muscle-derived stem cells in peripheral nerve regeneration [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1130-1136. |
| [5] | Zhang Jinglin, Leng Min, Zhu Boheng, Wang Hong. Mechanism and application of stem cell-derived exosomes in promoting diabetic wound healing [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(7): 1113-1118. |
| [6] | Li Shuo, Su Peng, Zhang Li, Wu Qiulong, Hu Xiangyu, Lai Yuliang. Positive effect of supracondylar femoral osteotomy on the correction of knee varus based on three-dimensional reconstruction and finite element analysis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(6): 858-863. |
| [7] | He Yunying, Li Lingjie, Zhang Shuqi, Li Yuzhou, Yang Sheng, Ji Ping. Method of constructing cell spheroids based on agarose and polyacrylic molds [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 553-559. |
| [8] | He Guanyu, Xu Baoshan, Du Lilong, Zhang Tongxing, Huo Zhenxin, Shen Li. Biomimetic orientated microchannel annulus fibrosus scaffold constructed by silk fibroin [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 560-566. |
| [9] | Chen Xiaoxu, Luo Yaxin, Bi Haoran, Yang Kun. Preparation and application of acellular scaffold in tissue engineering and regenerative medicine [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 591-596. |
| [10] | Kang Kunlong, Wang Xintao. Research hotspot of biological scaffold materials promoting osteogenic differentiation of bone marrow mesenchymal stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 597-603. |
| [11] | Shen Jiahua, Fu Yong. Application of graphene-based nanomaterials in stem cells [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 604-609. |
| [12] | Zhang Tong, Cai Jinchi, Yuan Zhifa, Zhao Haiyan, Han Xingwen, Wang Wenji. Hyaluronic acid-based composite hydrogel in cartilage injury caused by osteoarthritis: application and mechanism [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 617-625. |
| [13] | Li Hui, Chen Lianglong. Application and characteristics of bone graft materials in the treatment of spinal tuberculosis [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 626-630. |
| [14] | Gao Cangjian, Yang Zhen, Liu Shuyun, Li Hao, Fu Liwei, Zhao Tianyuan, Chen Wei, Liao Zhiyao, Li Pinxue, Sui Xiang, Guo Quanyi. Electrospinning for rotator cuff repair [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(4): 637-642. |
| [15] | Guan Jian, Jia Yanfei, Zhang Baoxin , Zhao Guozhong. Application of 4D bioprinting in tissue engineering [J]. Chinese Journal of Tissue Engineering Research, 2022, 26(3): 446-455. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||